Home » Blood pressure measurement
Hypertension is one of the most important preventable causes of premature morbidity and mortality. It can be defined as “elevation of the arterial blood pressure above the normal range expected in a particular age group”. There is a continuous independent relationship between usual blood pressure and incidence of cardiovascular events such as stroke, heart failure and death from vascular disease. Lowering blood pressure has been shown to reduce the risk of both cardiovascular and total mortality, without adverse effect on quality of life.
It is estimated that 950,000 (62.2%) adults aged 45+ in Ireland have high blood pressure. This estimate includes those adults with raised blood pressure who are unaware of their diagnosis, estimated to be some 595,000 adults. Given the number of undiagnosed cases of hypertension and the known benefits of therapy, diagnosis is important. The basis for diagnosing and managing hypertension is the measurement of blood pressure.
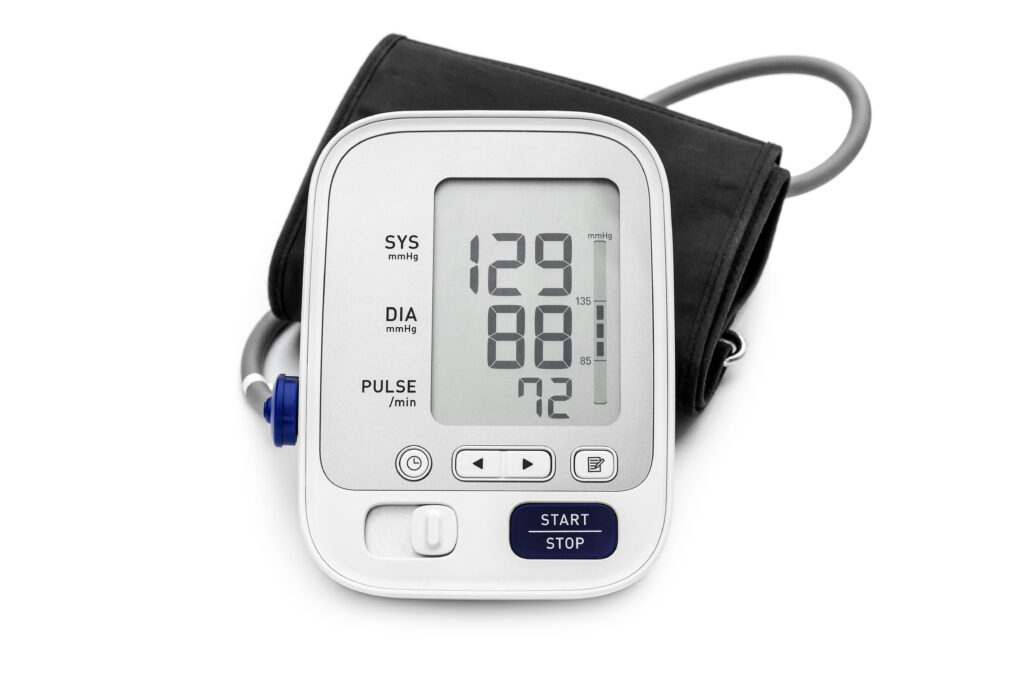
Blood pressure is measured in millimetres of mercury (mmHg) and is given as two figures:
Readings are displayed as systolic pressure/diastolic pressure.
There are a number of different types of blood pressure measurement. Blood pressure that is measured in a clinical setting such as in a hospital or by a doctor in general practice, is typically referred to as office blood pressure measurement. Ambulatory blood pressure measurement (ABPM), also known as 24-hour blood pressure measurement, involves monitoring blood pressure over a prolonged period, usually 24 hours. Repeated measurements taken at set intervals (usually every 30 minutes), provide a profile of blood pressure fluctuations over an entire day giving information on both daytime and, importantly, nighttime blood pressure patterns. Home blood pressure measurement refers to repeated measurements outside of the clinical setting, generally in a person’s own home, according to an agreed schedule. A typical schedule involves measurements taken twice daily (morning and evening), over a consecutive seven-day period and at a minimum for at least three days.
The 2021 European Society of Hypertension Practice Guidelines for Office and Out-of-office Blood Pressure Measurement provide a useful overview of recommendations in relation to blood pressure measurement. They highlight the importance of accurate methodology for measurement and the use of validated devices. Inadequate measurement techniques and/or the use of inaccurate machines can lead to overdiagnosis and overtreatment, or underdiagnosis and exposure to preventable cardiovascular disease.
Automated electronic devices are used frequently, and their use is almost exclusively in ambulatory and home blood pressure measurement, as well as in the community pharmacy setting. The use of a reliable device is essential, and in this respect, monitors that have been successfully validated by using an established validation protocol should be used. The British and Irish Hypertension Society maintains a list of validated monitors (see bihsoc.org > BP Monitors). Some monitors that are validated for use in adult populations may not be accurate in other populations (for example, children, pregnant women), and in these populations separate validation may be necessary.
There is a continuous independent relationship between usual blood pressure and incidence of cardiovascular events such as stroke, heart failure and death from vascular disease.
In order to ensure accurate blood pressure measurement, the selection of an appropriate cuff size is critical. Electronic monitors have their own cuffs, and they are not interchangeable with other devices. A cuff that is too small overestimates blood pressure, whereas one that is too large will overestimate it. The size to be chosen will depend on the arm circumference of the patient; where an automated electronic device is used the device will come with instructions as to what size cuff should be used for a set range of arm circumference values. Instructions on correct positioning on the arm should also be provided.
When taking a blood pressure measurement using an automated electronic device in the community pharmacy setting, there a few considerations to ensure an accurate measurement procedure:
Figure 1: Poster of OBP measurement methodology

Devices should be maintained to ensure good working order with annual maintenance, and/or recalibration as required, and as recommended by the manufacturer.
A diagnosis of hypertension should never be made on the basis of a single measurement. In some limited circumstances clinicians may diagnose hypertension where the blood pressure is very high (e.g. ≥180/110 mmHg), and there is evidence of target organ damage, or cardiovascular disease. However, in most cases the diagnosis should be confirmed by ambulatory or home blood pressure measurement. ABPM has a number of advantages over other methods of blood pressure measurement, such as the ability to provide detail on an individual’s usual level of blood pressure control outside the clinic setting, and over a twenty-four hour period, thus facilitating the diagnosis of patterns of blood pressure behaviour that are not readily identifiable by other means. Examples include:
Home blood pressure monitoring is widely available at a relatively low cost and can also detect white coat and masked hypertension. However, it does not provide any information on night-time patterns of blood pressure.
In the community pharmacy setting, blood pressure measurements can be used for screening and opportunistic detection with onward referral to a GP where measurements are found to be out of range.
The European Society of Cardiology classify blood pressure according to seated office blood pressure, and the classifications are outlined in Table 1.
Table 1: Categories for conventionally measured seated office blood pressurea. Reference, Visseren, FLJ, Mach F et al 2021 ESC Guidelines on cardiovascular disease prevention in clinical practice European Heart Journal (2021) 42, 32273337
| Category | SBP (mmHg) | DBP (mmHg) | |
| Optimal | <120 | And | <80 |
| Normal | 120-129 | and/or | 80-84 |
| High-normal | 130-139 | and/or | 85-89 |
| Grade 1 hypertension | 140-159 | and/or | 90-99 |
| Grade 2 hypertension | 160-179 | and/or | 100-109 |
| Grade 3 hypertension | >180 | and/or | >110 |
| Isolated systolic hypertensionb | >140 | And | >90 |
BP = blood pressure; DBP = diastolic blood pressure; SBP = systolic blood pressure.
aBP category is defined according to seated clinic BP and by the highest level of BP, whether systolic or diastolic.
bIsolated systolic hypertension is graded 1, 2, or 3 according to SBP values in the ranges indicated.
There are different blood pressure threshold levels for hypertension when ambulatory or home blood pressure measurements are used, with threshold values lower than for measurements taken in the clinic.
National policy recommends a shared care approach to cardiovascular disease risk assessment, and ongoing management in the primary care setting, with the role of both General Practice and pharmacy noted in this regard. The prevalence of hypertension is growing in tandem with increases in longevity. With the vast majority of hypertensive patients being managed in primary care, ready access to blood pressure measurement services in that setting is important. Addition of a pharmacy model thus complements existing service provision, as it removes barriers to screening by providing a service when others are inaccessible. Indeed, adoption of a shared care model where patients receive ABPM in their local community pharmacy with onward referral to their GP for diagnosis and therapy initiation, may facilitate more appropriate use of resources in primary care.
References available on request.
Susan O’Dwyer

Head of Governance and Pharmacy Services, IPU
Highlighted Articles